Chemo Complete, Surgery Behind Us, and Healing Ahead
I know it's been a long while since our last update, and as always, we are so grateful for everyone's patience, love, and continued support as they follow along on Dave’s journey.
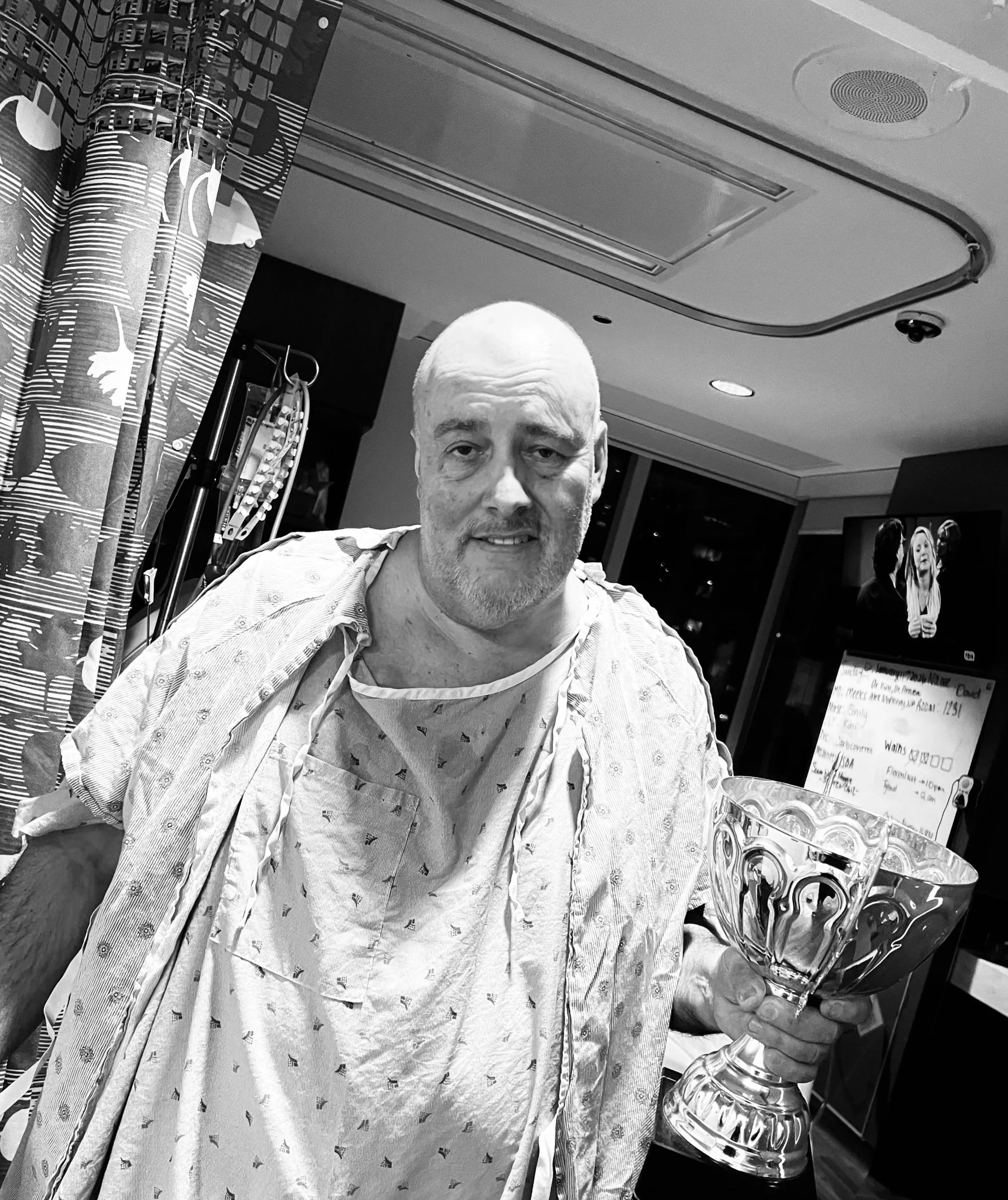
On December 9th, he completed his final round of chemotherapy. Reaching the end of chemo was a major milestone—one that came with endless exhaustion and a deep sense of gratitude. Chemo was not easy on his body, but he showed up each time with determination and grit, and kept most of his hairs! To celebrate, he was forcefully encouraged to ring the ceremonial end-of-chemo gong by his persuasive daughter!
Dave had just under four weeks to rest and “recover” before we trekked back downtown for the next step in his treatment. His surgery would entail the removal of his bladder, prostate, and lymph nodes in the groin. Once these are removed, the surgeon would resect a portion of the small intestine to create an ileal conduit (internal), connect the ureters to the conduit, and construct the stoma (external) to provide a permanent urinary diversion.
So, you know, an outpatient procedure if you talk to insurance (kidding)!
On Monday, January 5th, Dr. Meeks and the most talented team at Northwestern served the eviction notice on Dave’s bladder and its friends. He was taken back into the operating room at 2:30 pm, and his family immediately headed downstairs for Happy Hour margaritas (okay, mostly just his daughter). While Cheri received steady updates between 2:30 pm and 5:00 pm, the next scheduled update at 6:30 pm never came, and radio silence filled the hours between then and 8:30 pm. Now that we were completely convinced something had gone very wrong, we headed back up to an empty family surgical waiting room. Thankfully, they keep a phone on the counter with a number to call for moments such as this, and we promptly phoned in for a “Now, would be a good time to tell us he is fine” update. Minutes later, a nurse called from the operating room, saying he was doing well and that they hoped to close up in the next 30 minutes.
Like clockwork, Dr. Meeks (A.K.A. the best surgeon in the world) called to give us a post-surgical update on Dave.
As they began Dave’s surgery, they realized that part of his bowel and small intestine had grown into the mesh that was placed during a hernia surgery twenty-five years earlier. Because we have access to some of the best doctors science has to offer, Dr. Meeks brought in a specialty surgeon who spent over an hour and a half separating his bowel and intestines from the mesh. After that unexpected delay, his planned surgery moved forward and was without complication!
Coming out of anesthesia after seven hours of surgery was rough. The pain was unbearable, made torturous by the plot twist that he wasn’t going to receive any narcotic pain relief. Dave had lost two organs, six nodes, had four incisions, and was put on a less-than-mediocre intravenous Tylenol drip.
The next seven days in the hospital were defined by pain, very little sleep, and the slowest possible relationship with food. Water only. Then chicken broth. Then cream of chicken soup. Then back to water. For days, he bounced between the two, unable to consistently tolerate even a “full liquids diet.” Progress was measured in Italian ice.
On night six, Erica stayed overnight at the hospital to more directly confront the rotating team of residents and providers about his pain management. Her sleepover included teaching a resident some long-overdue people skills, chicken meatballs from Beatrix Market, and—finally—on the morning of day seven, her 35th birthday, Dave was started on oral oxycodone every four hours.
Being told that Dave was the first of Dr. Meeks’ patients to ever receive narcotics after this surgery was the best birthday gift Erica could have asked for; challenge accepted, and won.
Days seven through ten were a mix of ups and downs: trying to get ahead of the pain instead of chasing it, getting a little more rest, discovering truly wild bruising everywhere, leaning hard on incredible nurses and techs, expanding the menu to include more liquid and semi-solid liquid-adjacent foods, walking constantly, and stealing a trophy from the nurses’ station for said walking.
It was thrilling when Dave, in his own words, “found something to live for” on day nine, though his wife and children were mildly disappointed to learn that thing was Cream of Wheat. 😂
Once he had made all the progress the hospital could offer, we made plans to bring him home. Dave was discharged late Wednesday, January 14th. Since then, we’ve been figuring out comfort, calories, and routines, with the help of a nurse who comes to the house three times a week.
We’ll be back soon with another update on how life at home is going, along with next steps based on the pathology results from surgery.